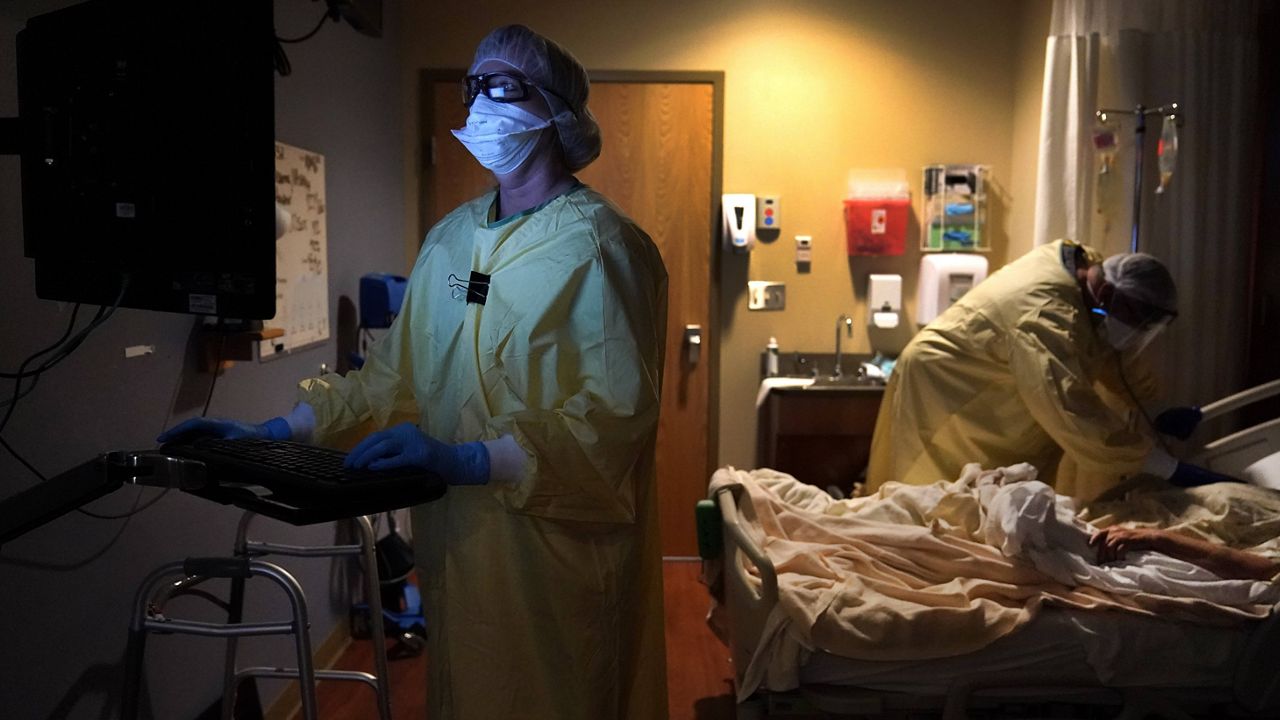
For health care workers in the coronavirus pandemic, some cases are harder to shake. For Kiersten Henry, it was a father of two in his 50s.
What You Need To Know
- Many nurses across the country say they’re dealing with extreme stress related to the pandemic, which could lead to PTSD
- A Yale School of Public Health study found that one in four health care workers were experiencing PTSD
- Repeated exposure to trauma as well as feelings of helplessness, lack of PPE and fear of contracting the virus are contributing to nurses' stress
- Among the effects of PTSD are nightmares, insomnia, emotional numbing or withdrawal and substance abuse
Henry, an intensive care nurse practitioner at MedStar Montgomery Medical Center in Olney, Maryland, was part of a team that fought for more than a month to treat the man, but it eventually became clear he would not recover. His wife and daughter were by his side to say goodbye; his young son had one last FaceTime call with him.
"It just leaves everybody feeling defeated,” Henry said. “We want to make people better. You just feel helpless that you can't make these people better and that you're doing everything that you can, and you're just watching them get worse."
Henry is among the many nurses across the country who say they’re dealing with extreme stress related to the pandemic. However, she shies away from using the term “post-traumatic stress disorder,” or PTSD, noting, “I still think we're in the middle of it.”
"I think it would be fair to say all of us have some degree at this point of moral distress around this,” she said. “But I think that none of us feel like we're past it to even know how it's going to feel to be post this sort of ongoing trauma."
Nevertheless, the novel coronavirus has made post-traumatic stress disorder, as well as other mental health issues, very real concerns for health care workers, including nurses.
While the true scope of the problem won’t be known for some time, a Yale School of Public Health study of 1,132 health care workers from 25 medical centers published in late October found that about one in four was experiencing PTSD, while many others said they were battling major depression, anxiety disorder or alcohol abuse.
Another recent survey conducted by the magazine Nursing Standard found that eight in 10 nurses who responded said their mental health has been affected by the pandemic, with some reporting symptoms of PTSD.
According to the American Psychiatric Association, PTSD can be triggered by direct and indirect exposure to traumatic events. It’s something health care workers must contend with even outside the pandemic, but the heavy and seemingly never-ending COVID-19 caseloads are exacerbating the problem in 2020.
“Sometimes we consider some of that secondary PTSD or vicarious trauma because you're observing it happening to others often, and that can contribute to something called compassion fatigue, which it just takes an emotional and then a physical toll on the body because it can produce the same effects as PTSD,” Diane Esposito, a psychiatric advanced practice registered nurse and an associate professor at Palm Beach Atlantic University, told Spectrum News.
Also contributing to the stress, health experts say, is the helplessness health care workers feel, the lack of personal protective equipment and the fear of contracting the virus, and the added pressure felt to comfort patients when loved ones are not allowed into hospital rooms. Nurses also are simultaneously dealing with the same concerns at home that countless other families are, including spouses being out of work and children attending school remotely.
“During the pandemic, nurses have been asked to work longer hours, they are caring for some of the sickest patients they’ve ever cared for in large numbers and taking on a larger assignment (more patients per shift) than usual,” Marian Altman, a clinical practice specialist for the American Association of Critical-Care Nurses, said in an email to Spectrum News.
“Nurses are witnessing suffering and experiencing moral distress like never before. Patients are dying without their families and significant others present with them and nurses are feeling the pressure to be there in their absence,” she added.
PTSD cannot be diagnosed until six months after symptoms develop, and the effects could be short-term or chronic. Experts say those symptoms can include adverse effects to someone’s mental, physical and spiritual well-being; nightmares; insomnia; feeling on edge; avoidance; and emotional numbing or withdrawal.
Sometimes those dealing with PTSD turn to substance abuse. And extreme cases could lead to suicide — a worsening problem in the medical world even before the pandemic, studies show.
"I think, as a group, nurses are very resilient, but they also tend to focus more on helping others — obviously that's why they became a nurse and they're caring and wanting to help others — but sometimes it could be at the expense of themselves or their own self-care,” Esposito said.
PTSD is most commonly associated with soldiers returning from war. And for that reason, nurses are reluctant to describe what they’re experiencing as PTSD, Henry said. But there are some undeniable parallels, especially related to the COVID-19 crisis.
“This is the first time we go to work and we worry about, is this the day that I get sick? Is this the day one of my colleagues gets sick, and potentially fatally ill?” said Henry, who is also an AACN board member. “So it's very much different than combat, but I think it's the first time that we as a profession have faced that kind of front-line danger day in and day out.”
Henry said there just isn’t enough time right now for nurses to heal emotionally between patients dying.
“When you lose a patient or it's a traumatic death, it has an impact,” she said. “But usually you can kind of go home, recover from that, you have a couple of good patient stories that help fill your cup a little and you have more time before the next one. And now it's like this relentless onslaught."
Many hospitals have been focusing for months on ways to help health care workers struggling mentally. Some ways to help mitigate or treat stress include encouraging self-care — such as relaxation therapy, yoga or exercise — establishing support systems and offering counseling and medication.
Nurses are also leaning on each other more. Henry said one approach her team has taken is to participate in “end-of-shift huddles” to share positives from an otherwise trying day. The goal is to boost morale.
But she added the bigger problem can’t be confronted until health care workers first acknowledge it.
“The first step is saying, 'This sucks,' and, ‘Hey, I didn't want to come to work today,’ or, ‘I sat in my car an extra two minutes to work up the energy to come in today ’cause I'm just tired.’"
And nurses say the general public can do their part, too, by taking COVID-19 precautions seriously to help prevent hospitals from becoming overwhelmed, feeding the vicious cycle that wears on health care professionals.
“It is devastating to healthcare professionals to see people blatantly ignore safety precautions that are proven to slow the spread of this virus in our communities while they work 24/7 to deal with the havoc produced by this pandemic,” Altman wrote.